Health Essentials
Urinary tract infection is common, do not take it home!

Have you ever experienced a burning sensation while urinating? Did your urine have a strong smell? Were you also experiencing frequent urination at the time?
Then you may have had a Urinary Tract Infection. The above symptoms are but a few of the symptoms if it presents any.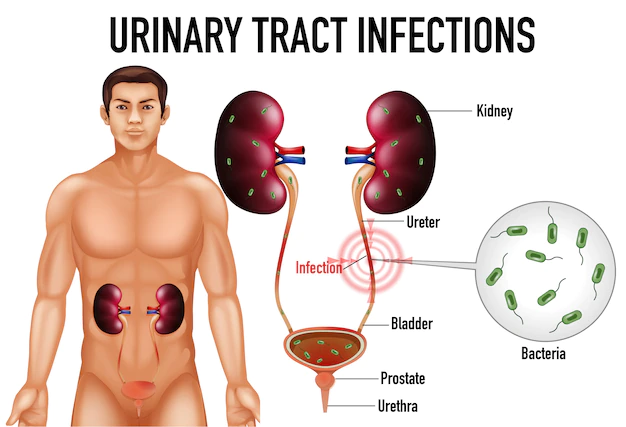
Urinary tract infections (UTIs) can occur in any part of your urinary tract – kidneys, ureters, bladder, or urethra. Infections of the lower urinary tract – the bladder and urethra – are most common.
Women are more likely to experience UTIs than men. Infections of the bladder can be uncomfortable and unpleasant, but if a UTI spreads to your kidneys, serious consequences can occur.
There are not always symptoms associated with urinary tract infections, but when they do occur they may include:
- A strong, persistent urge to urinate
- Burning sensations when urinating
- Routinely passing small amounts of urine
- Cloudy urine
- Blood in the urine may appear red, bright pink, or cola-coloured
- Strong-smelling urine
- A woman may experience pelvic pain, especially in the area of the pubis
Elderly adults are more likely to overlook UTIs or confuse them with other conditions.
Infections can occur in different parts of the urinary tract, and they are called by different names depending on where they happen.
- Cystitis of the bladder can cause you to pee excessively or to feel pain when you do. It can also cause you to have cloudy urine or blood in your urine.
- Pyelonephritis (kidneys) can result in fever, chills, nausea, vomiting, and upper back pain and discomfort.
- Urethritis may cause a discharge and pain when you urinate.
Bacteria entering the urinary tract through the urethra and multiplying in the bladder often cause urinary tract infections. Even though the urinary system is designed to protect against such bacteria, these defences sometimes fail. If that occurs, bacteria could take hold and grow into a full-blown infection in the urinary tract.
- Infection of the bladder (cystitis). In this type of UTI, Escherichia coli (E. coli), a type of bacteria commonly found in the gastrointestinal tract (GI), is responsible for the infection. However, other bacteria can also cause infection. Sexual intercourse may lead to cystitis, but you don’t have to be sexually active to develop it. A woman’s anatomy makes her vulnerable to cystitis, especially the short distance between the urethra and anus and the opening along the urethral wall that leads to the bladder.
- Infection of the urethra (urethritis). In this type of UTI, GI bacteria spread from the anus to the urethra. Additionally, because the female urethra is located close to the vagina, infections such as herpes, gonorrhoea, chlamydia, and mycoplasma may cause urethritis.
Women are prone to urinary tract infections, and many experience more than one infection in their lifetime. Specific risk factors for women include:
- Female anatomy. Women have a shorter urethra than men, which makes it easier for bacteria to reach the bladder.
- Sexual activity. Women who are sexually active tend to have more UTIs than those who aren’t. Switching partners also increases your risk.
.
- Birth control methods. Women who use diaphragms for birth control, as well as those who use spermicidal agents, may be at higher risk.
- Menopause. As estrogen levels decline during menopause, you become more susceptible to infections in the urinary tract.
- Abnormalities of the urinary tract. The risk of UTIs is higher in babies born with abnormalities of the urinary tract that prevent urine from leaving the body normally or cause urine to back up in the urethra.
- Urinary tract obstructions. UTIs can be caused by kidney stones or an enlarged prostate that trap urine in the bladder.
- A suppressed immune system. The risk of UTIs increases with diabetes and other diseases that impair the immune system.
- Catheter use. An increased risk of UTIs exists for people who can’t urinate on their own and use a tube (catheter). The category may include people who are hospitalised, people with neurological problems that make it hard for them to control their bladder function, and people who are paralysed.
- Recent urological surgery. An exam of your urinary tract with medical instruments or a surgery on your urinary tract can both place you at risk for urinary tract infections.
Infections of the lower urinary tract rarely result in complications when they are treated promptly and properly. An untreated urinary tract infection, however, can cause serious complications.
Complications of a UTI may include:
- Recurring infections, especially in women who experience more than two UTIs in a six-month period or four or more within a year.
- Acute or chronic kidney infection (pyelonephritis) caused by an untreated UTI that permanently damages the kidneys.
- Pregnant women are more likely to deliver low birth weight or premature babies.
- Men with recurrent urethritis have narrowing (stricture) of the urethra, a condition previously seen with gonococcal urethritis.
- Infections can lead to sepsis, which is a potentially life-threatening complication, especially if the infection goes into your urinary tract or kidneys.
Here are some steps you can take to reduce your risk of urinary tract infections:
- Drink plenty of liquids, especially water. Drinking water helps dilute your urine and ensures that you’ll urinate more frequently — allowing bacteria to be flushed from your urinary tract before an infection can begin.
- Drink cranberry juice. Although studies are not conclusive that cranberry juice prevents UTIs, it is likely not harmful.
- Wipe from front to back. Doing so after urinating and after a bowel movement helps prevent bacteria in the anal region from spreading to the vagina and urethra.
- Empty your bladder soon after intercourse. Also, drink a full glass of water to help flush bacteria.
- Avoid potentially irritating feminine products. Using deodorant sprays or other feminine products, such as douches and powders, in the genital area can irritate the urethra.
- Change your birth control method. Diaphragms, or unlubricated or spermicide-treated condoms, can all contribute to bacterial growth.
Source:
Maureen Masopeh and Tina Amarh
Content Creators
Health Essentials Ghana Limited
References:
- Mayoclinic.org
- Webmd.com
By Dr. Kojo Cobba Essel
Health Essentials
Identifying the geriatric giants & taking appropriate steps

This week I bumped into Deborah, one of my avid readers and I promised her I will be writing this weekend. So Deborah, this is for your reading pleasure and to pick some golden nuggets for the future.
The quest to find the best way to make one’s golden years, happy, exciting, healthy and a time most people look forward to continues unabated. One factor that keeps popping up is the need to grow friendships with people more than 20 years younger than yourself.
Do not take this for granted. It is a form of “social security” since these close friends who are much younger than you will step in to support you in more ways than you can ever imagine.
Some conditions may make life challenging for older adults but knowing these Geriatric Giants helps us to take the necessary steps to reduce our risk.
“Geriatric Giants” refers to a group of chronic health conditions that are common in the elderly, typically 65-year-olds and older.
These conditions quite often co-occur and can impact on the independence, dignity and overall wellbeing and quality of life of an elderly person.
These Geriatric Giants include:
- Impaired Intellect/ Memory (e.g. Dementia)
- one of the major battles we need to deal with is challenges with memory
- Exercise, adopt the Mind Diet, build a great social network and enjoy time outdoors
- Keep reading and solving puzzles for as long as possible
- Instability – leading to much feared falls
- A good reason to indulge in Balance Training and Core Strengthening exercises from today
- Ensure your home is safe; avoid clutter such as cables crisscrossing floors, toys etc. These are all trip hazards and should be avoided
- Many healthy, happy and fun-loving older adults have died soon after a fall with its attendant complications.
- Do whatever it takes to avoid falling
- Immobility (opening the doors to pressure sores, joint stiffness)
- Even when you are unable to move about on your own it is important to get support to change positions as often as possible or get an appropriate mattress or bed that prevents prolonged pressure over any single point.
- Make sure you passively or actively move joints daily.
- Incontinence (urine, faeces or both)
- This is one of the reasons older adults prefer to stay at home and avoid going out to meet friends etc.
- Iatrogenic Disorders – adverse effect of medication
- Quite often most older adults are on several medications and some side effects such as drowsiness may seem to cause more unhappiness and may even lead to falls.
- Inappetite – this may result in poor nutrition
- This may also be linked to loss of teeth thus making chewing very difficult or limited.
- The loss of smell and taste may also reduce the amount of food one may willingly eat.
The power to reduce the impact of the Geriatric Giants starts now and should be a lifetime commitment. It is never too early to start making the appropriate lifestyle modifications, nor is it too late to reduce the impact of the giants on one’s life.
Other conditions that significantly impact on the lives especially of the elderly are:
- Sleep Disorders
- Good sleep has the power to give us energy, improve our thought pattern and even helps us to make good choices.
- Good sleep sets the tone for a healthy life
- Constipation
- This is a challenge that confronts quite a number of older adults.
- Movement, fibre and lots of water go a long way to reduce the stress that frequent constipation generates.
- Fraility
- Muscle loss is real and as we age, we lose a significant percentage of our muscle plus our bones also become brittle.
- Make sure strength training is part of your exercise schedule
- Polypharmacy
- Another headache that needs to be confronted head-on
- Everyone especially older adults need a good primary care physician or a general practitioner who can coordinate all medicines from the different Specialists who may be attending to an elderly person. This ensures that unnecessary medicines are dropped
The goal of care at all times is to optimise the quality of life. As family, professional caregivers and friends we should always show respect so that the dignity of the elderly is preserved at all times. For those of us who are not yet in the age group with such challenges, we need to start the conversation about the type of care we will prefer and take steps to stay healthy and independent for as long as possible. The goal should be a long Healthspan and not just a long Lifespan.
AS ALWAYS LAUGH OFTEN, ENSURE HYGIENE, WALK AND PRAY EVERYDAY AND REMEMBER IT’S A PRICELESS GIFT TO KNOW YOUR NUMBERS (blood sugar, blood pressure, blood cholesterol, BMI)
Dr. Kojo Cobba Essel
Health Essentials Ltd (HE&W Group)
(dressel@healthessentialsgh.com)
*Dr. Essel is a Medical Doctor with a keen interest in Lifestyle Medicine, He holds an MBA and is an ISSA Specialist in Exercise Therapy, Fitness Nutrition and Corrective Exercise. He is the author of the award-winning book, ‘Unravelling The Essentials of Health & Wealth.’
Thought for the week – “There is no magic formula to being happy but making a conscious effort to be happy goes a long way.” – Dr. Kojo Cobba Essel
By Dr. Kojo Cobba Esse
Health Essentials
Why Ghana’s ‘no bed syndrome’ is a policy failure, not a clinical failure -Part 2

The call to action
We must move beyond the cycle of temporary outrage. I propose a four-point blueprint for the Ministry of Health and the government:
1. A Digital Bed-Tracking Command Centre: Legally mandate all public and major private hospitals to update a live, digital bed-registry every hour. The NAS must be able to see a vacancy before they move. This must be matched with the available resources and services so that the right patient will be sent to the right facility.
2. Strategic Capacity Expansion: We must stop building “prestige projects” and start building high-volume stabilisation centres. We need a targeted investment to triple the ER bed count in Accra and Kumasi within 24 months. This should then be extended to other regional capitals.
3. Specialised Emergency Hubs: Designate specific hospitals as “Centres of Excellence” for Cardiac and Stroke care (and for other health emergencies), ensuring they have 24/7 imaging and intervention capabilities as well as the requisite expertise to manage these conditions. Policy makers must incentivise public-private partnerships to ensure that a heart attack in Accra or Kumasi can be treated with the same urgency as one in New York.
4. Develop a nationwide trauma system: This is extremely important because trauma is a major cause of deaths in Ghana. In the US, each state has a statewide trauma system with three levels. Level 1 trauma centres are usually University Teaching hospitals that provide comprehensive trauma care and also play an important role in local trauma system development, regional disaster planning, increasing capacity and advancing trauma care through research. Level II trauma centres are expected to provide initial definitive trauma care for a wide range of injuries and injury severity.
Level III centres provide definitive care to patients with mild trauma. Having such systems is imperative to ensure proper treatment of trauma patients.
Even for those who survive trauma, disability is a major assault on economic potential and viability. Importantly all this cannot happen with a cash and carry system. Emergencies should be managed under a different model to save life and limb first. Obviously, there is a need to ensure that healthcare facilities will be able to recover their investments in emergency care, and that balancing act needs careful consideration.
Frontline clinicians are often forced to bear the public’s anger for infrastructure deficits they did not create and cannot fix. This is a failure of governance, not a lack of clinical care. Responsibility lies with the policy makers who manage the nation’s resources.
The “No Bed Syndrome” is a systemic disease. It cannot be cured with a directive from the Ministry of Health, parliament or a lecture on ethics. It requires a blueprint, a budget, and the political will to treat this like the menacing threat it is.
It is safe to say that non-emergent healthcare is excellent in Ghana for the most part if you can afford it. However, emergency care is suboptimal. We had a sitting president die from an emergency health issue and a former vice president also die from an emergency. If that is not enough warning, it is clear that anyone can be a victim of an emergency.
If we do not act, the next ambulance driving aimlessly through the streets of Accra could be carrying anyone, including the very people who have the power to fix this issue.
Prof. Jonathan Laryea is a Professor of Surgery at the University of Arkansas for Medical Sciences in Little Rock. Arkansas. He is board certified in General Surgery, Colorectal Surgery and Clinic Informatics.
He is a graduate of the University of Ghana Medical School (Class of 1997)

 News3 days ago
News3 days agoGhana’s Chris Koney participates in high-level dialogue at Africa Forward Summit 2026

 News1 week ago
News1 week agoIsaac Adongo defends BOG Governor, says Ghana “in safe hands”

 Features3 days ago
Features3 days agoFix It Fast or Lose Them Forever: The Ever-Rising Importance of Service Recovery in Competitive Industries







