Health Essentials
Combating heartburn & fire in your belly at Christmas & beyond
Over the past few months I have noticed a worrying trend of people getting repeated episodes of heartburn as well as unbearable burning sensation in their bellies. Many of the “victims” seem to be in a long-term relationship with nonsteroidal anti-inflammatory painkillers such as ibuprofen and are often in love with high dose dispersible Vitamin C as well as lemon, spices and a host of other concoctions.
There seems to be a link with COVID-19 in this surge and especially in people who claim they had been diagnosed with peptic ulcer disease but had been perfectly fine for decades.
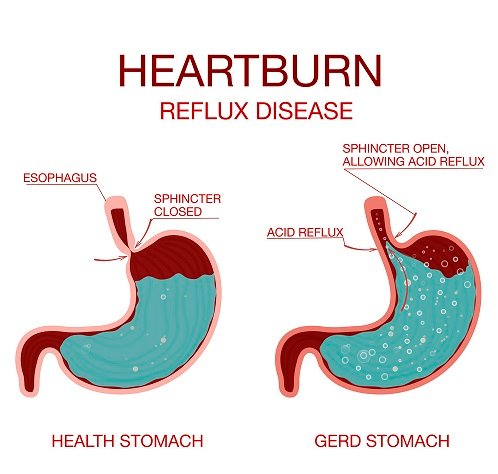
Peptic Ulcer Disease is commonly caused by long-term NSAID use and infection by the bacterium Helicobacter pylori (H. pylori). All other factors such as spices, cigarette smoking and caffeine consumption do not cause the ulcer BUT aggravate/ worsen the symptoms. In reflux disease referred to as “heartburn”, the band at the junction of the stomach and oesophagus (tube from throat into stomach) is weak so allows stomach contents including acid back “upstairs” where they have no business.
Quite often many people tend to self-diagnose and treat with a few bottles of an antacid and may even add prescription medication for about two weeks. Do get professional assistance because not treating peptic ulcer or reflux disease appropriately may mean years of pain and distress and even in a few instances things may progress to life-changing situations.
Our focus in this interaction is to assume you are being properly managed for your reflux disease and peptic ulcer disease. We will share lifestyle changes that are critical in speeding up the healing process and in many instances keeping it at bay for years. You surely will be thankful at least for an end to poor sleep, disturbing cough and what may appear to be an adult onset asthma together with many more.
DO THESE IN ADDITION TO WHAT YOUR DOCTOR PRESCRIBED:
1. Keep a Food Diary and keep a record of anything that you eat or drink that triggers pain in your chest or belly. This is helpful because the guidelines we give work for most people but you may have things that are peculiar to you and ONLY a food diary will unearth that.
2. Eating a balanced meal that contains vegetables, fruits and whole grains
3. Avoid nonsteroidal anti-inflammatory drugs (NSAIDs) for managing pain. These include diclofenac, ibuprofen etc. To be safe paracetamol/Panadol/Tylenol should be what you go for except when your health professional who is aware of your condition advises otherwise
4. Taking a multivitamin. This is because a vitamin or other nutrient deficiency makes healing of ulcers difficult
5. In the treatment phase I suggest you avoid alcohol
6. Do not smoke cigarettes and do not inhale (passive smoker) it either
7. Avoid caffeine in tea and coffee
8. Avoid caffeine from other sources such as chocolate and other drinks
9. Avoid fizzy drinks
10. Avoid spicy foods, which means pepper, ginger, nutmeg, onions, garlic etc. should be taken in very small quantities. I have seen tomato come up in the list of foods to avoid but I have found it difficult to understand. If you have issues when you take tomatoes then do reduce that as well but that leaves you with very few choices so I hope your food diary does not come up with tomatoes.
11. Avoid citrus fruits such as lemon, lime, oranges especially on an empty stomach
12. Be careful with fatty foods such as fried foods and most fast foods. I suggest dinner should not have fatty or “oily” foods at all especially if you belong to the heartburn squad.
a. Delicacies such as kelewele and khebab may be spicy and oily at the same time
13. Eat small frequent meals. Large meals have a way of waking up “sleeping dogs”
14. Peppermint or even drinks with the flavour tend to cause discomfort in some people. Avoid.
15. Your last meal should be at least three hours before sleep or DO NOT lie down for at least three hours after a meal
16. Keep active so you are healthy and reduce belly fat
17. Manage Stress; it exaggerates everything. Exercise, sleep, meditate, stay positive, be happy, get sunlight, show gratitude, give and give and give, get a hobby, spend time in the sun and close to nature. No one has all the answers to managing stress (a necessary evil).
Following your doctor’s treatment regime that may include antibiotics if you have H. pylori and taking some prescription medication for up to eight weeks together with these lifestyle modifications will go a long way to bring peace to your belly and quench the fire in your chest during this festive season and beyond.
AS ALWAYS LAUGH OFTEN, ENSURE HYGIENE, WALK AND PRAY EVERYDAY AND REMEMBER IT’S A PRICELESS GIFT TO KNOW YOUR NUMBERS (blood sugar, blood pressure, blood cholesterol, BMI)
Dr. Kojo Cobba Essel
Health Essentials Ltd/ Mobissel
(dressel@healthessentialsgh.com)
*Dr. Essel is a medical doctor, holds an MBA and is ISSA certified in exercise therapy, fitness nutrition and corrective exercise. He is the author of the award-winning book, ‘Unravelling The Essentials of Health & Wealth.’
Thought for the week –“A good FOOD DIARY includes everything that goes into your mouth, where you eat or drink, who you eat with and even your mood while you do that. It goes a long way to help you find the triggers to several challenges you may have.”- Dr. Kojo Essel
References:
1. Unravelling the Essentials of Health & Wealth; Dr. Kojo Cobba Essel
By Dr. Kojo Cobba Essel
Health Essentials
…Tips on building a healthy relationship with your superior
A good relationship with your boss is critical for job success and career development. Supervisors have a great influence on your stress level, your team and company culture, and ultimately, whether you succeed or fail in a role.
They are also your best resource for support, problem-solving, and personal development. Building a strong relationship with them can be transformative for your work experience and professional growth, but navigating this connection can be complex.
Here are some key values and characteristics that will help you along the way.
- Be authentic
It is important to be yourself when building any new relationship. Do not be over-the-top trying to impress or kiss up to a manager. Be authentic and try to build a genuine connection with them instead. This will be incredibly helpful when it comes to dealing with personal issues, having difficult conversations, and building trust.
- Be empathetic and respectful
Bosses are human beings with their own professional pressures and personal lives, so it is important to maintain empathy toward them. Strive to get to know them on a personal level; you do not need to be best friends, but knowing the basics, like their family and hobbies, can be meaningful.
Also, help your supervisor look good. Every leader wants a high-performing and successful team. By developing trust, understanding, and excellent communication, you can help your boss achieve their goals.
- Build trust and add value
Showing initiative will win you big points with almost any boss. Whether setting up regular one-on-ones, volunteering for new projects, or offering help, the benefits of this dedication are twofold.
Proactivity makes leaders feel supported-like you are looking out for them. It also provides opportunities for your individual growth.
Whenever possible, add value beyond the limitations of your job description. Whether you have a special interest or extra capacity, find ways to support your team and relieve pressure. – Source:careers.vikingservice.com
..To be continued
Health Essentials
Identifying the geriatric giants & taking appropriate steps

This week I bumped into Deborah, one of my avid readers and I promised her I will be writing this weekend. So Deborah, this is for your reading pleasure and to pick some golden nuggets for the future.
The quest to find the best way to make one’s golden years, happy, exciting, healthy and a time most people look forward to continues unabated. One factor that keeps popping up is the need to grow friendships with people more than 20 years younger than yourself.
Do not take this for granted. It is a form of “social security” since these close friends who are much younger than you will step in to support you in more ways than you can ever imagine.
Some conditions may make life challenging for older adults but knowing these Geriatric Giants helps us to take the necessary steps to reduce our risk.
“Geriatric Giants” refers to a group of chronic health conditions that are common in the elderly, typically 65-year-olds and older.
These conditions quite often co-occur and can impact on the independence, dignity and overall wellbeing and quality of life of an elderly person.
These Geriatric Giants include:
- Impaired Intellect/ Memory (e.g. Dementia)
- one of the major battles we need to deal with is challenges with memory
- Exercise, adopt the Mind Diet, build a great social network and enjoy time outdoors
- Keep reading and solving puzzles for as long as possible
- Instability – leading to much feared falls
- A good reason to indulge in Balance Training and Core Strengthening exercises from today
- Ensure your home is safe; avoid clutter such as cables crisscrossing floors, toys etc. These are all trip hazards and should be avoided
- Many healthy, happy and fun-loving older adults have died soon after a fall with its attendant complications.
- Do whatever it takes to avoid falling
- Immobility (opening the doors to pressure sores, joint stiffness)
- Even when you are unable to move about on your own it is important to get support to change positions as often as possible or get an appropriate mattress or bed that prevents prolonged pressure over any single point.
- Make sure you passively or actively move joints daily.
- Incontinence (urine, faeces or both)
- This is one of the reasons older adults prefer to stay at home and avoid going out to meet friends etc.
- Iatrogenic Disorders – adverse effect of medication
- Quite often most older adults are on several medications and some side effects such as drowsiness may seem to cause more unhappiness and may even lead to falls.
- Inappetite – this may result in poor nutrition
- This may also be linked to loss of teeth thus making chewing very difficult or limited.
- The loss of smell and taste may also reduce the amount of food one may willingly eat.
The power to reduce the impact of the Geriatric Giants starts now and should be a lifetime commitment. It is never too early to start making the appropriate lifestyle modifications, nor is it too late to reduce the impact of the giants on one’s life.
Other conditions that significantly impact on the lives especially of the elderly are:
- Sleep Disorders
- Good sleep has the power to give us energy, improve our thought pattern and even helps us to make good choices.
- Good sleep sets the tone for a healthy life
- Constipation
- This is a challenge that confronts quite a number of older adults.
- Movement, fibre and lots of water go a long way to reduce the stress that frequent constipation generates.
- Fraility
- Muscle loss is real and as we age, we lose a significant percentage of our muscle plus our bones also become brittle.
- Make sure strength training is part of your exercise schedule
- Polypharmacy
- Another headache that needs to be confronted head-on
- Everyone especially older adults need a good primary care physician or a general practitioner who can coordinate all medicines from the different Specialists who may be attending to an elderly person. This ensures that unnecessary medicines are dropped
The goal of care at all times is to optimise the quality of life. As family, professional caregivers and friends we should always show respect so that the dignity of the elderly is preserved at all times. For those of us who are not yet in the age group with such challenges, we need to start the conversation about the type of care we will prefer and take steps to stay healthy and independent for as long as possible. The goal should be a long Healthspan and not just a long Lifespan.
AS ALWAYS LAUGH OFTEN, ENSURE HYGIENE, WALK AND PRAY EVERYDAY AND REMEMBER IT’S A PRICELESS GIFT TO KNOW YOUR NUMBERS (blood sugar, blood pressure, blood cholesterol, BMI)
Dr. Kojo Cobba Essel
Health Essentials Ltd (HE&W Group)
(dressel@healthessentialsgh.com)
*Dr. Essel is a Medical Doctor with a keen interest in Lifestyle Medicine, He holds an MBA and is an ISSA Specialist in Exercise Therapy, Fitness Nutrition and Corrective Exercise. He is the author of the award-winning book, ‘Unravelling The Essentials of Health & Wealth.’
Thought for the week – “There is no magic formula to being happy but making a conscious effort to be happy goes a long way.” – Dr. Kojo Cobba Essel
By Dr. Kojo Cobba Esse







